Presentation Summaries: Day 1
2021 MASCC/ISOO Annual Meeting: Presentation Summaries
Presentation Summary Slide Set
Prepared by LeCancer.fr
Efficacy of cannabis in the management of anorexia? A Canadian study
Could cannabis be a solution to anorexia? This is the question that a Canadian study is trying to answer.
In view of the impact of the nutritional status of cancer patients on their quality of life, survival and health care costs, it seems necessary to define an effective management strategy for anorexia.
Tetrahydrocannabinol (THC) has an orexigenic effect. It appears that it may also have a beneficial effect on dysgeusia and dysosmia. However, the data in the scientific literature are limited and the conclusions are not yet significant. Thus, the Québec Cannabis Registry was used for a prospective, multicenter study, conducted between 2015 and 2018, in the province of Québec, to investigate the efficacy of medical cannabis in the treatment of anorexia.
Eighty-one out of 2991 patients were included in the registry. Appetite assessment was performed at inclusion and at 3 and 6 months with the ESAS appetite scale (revised). This database allows the definition of many demographic characteristics of the population studied. (See Fig. 1).
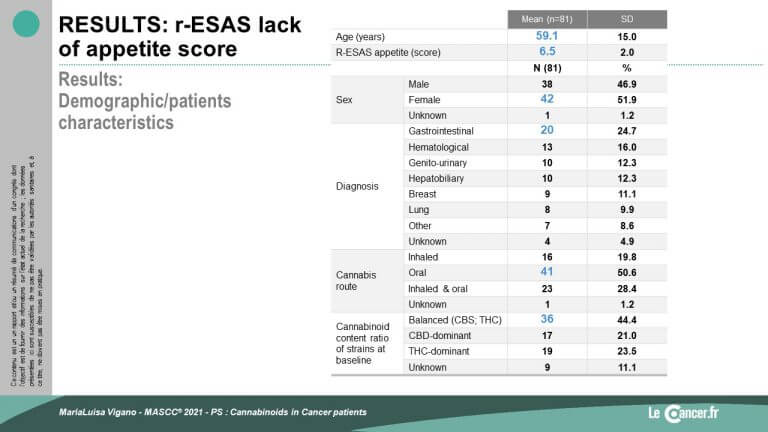
This study shows that the decrease in appetite loss is significant at 6 months (r-ESAS at 6.5 <4) and that 74% of patients show an improvement in their appetite (see Figs. 2 and 3).
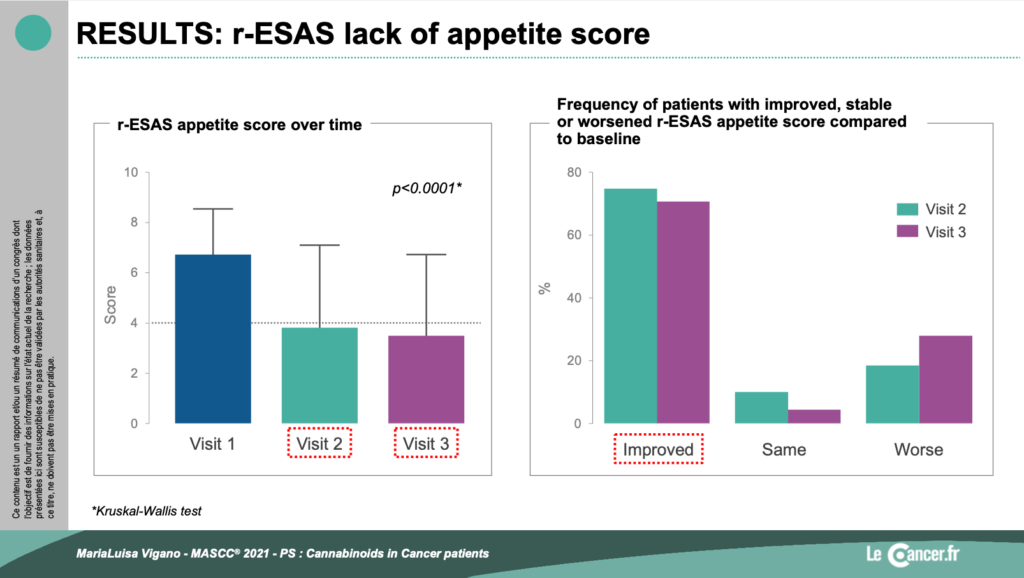
This demonstrates the value of medical cannabis in the management of anorexia in cancer patients but would need to be extended with a randomized study versus placebo and an evaluation of quality of life. Furthermore, this use should be under medical supervision to avoid any interaction with treatments. This underlines the importance of the quality of communication and the space of trust that must be created between the patient and the oncologist or advanced practice nurse.
Vigano ML. “Medical Cannabis to Relieve Anorexia in Cancer Patients: Results from a Canadian, Population-Based Study.” MASCC/ISOO 2021 Annual Meeting.
Undernutrition and cancer: How to act in practice?
Malnutrition and its advanced stage cachexia are a daily problem in clinical practice for cancer patients. Recognizing malnutrition, and where possible preventing it, is essential. This training session provided an update on this topic, covering all aspects from pathophysiology, diagnosis and treatment options.
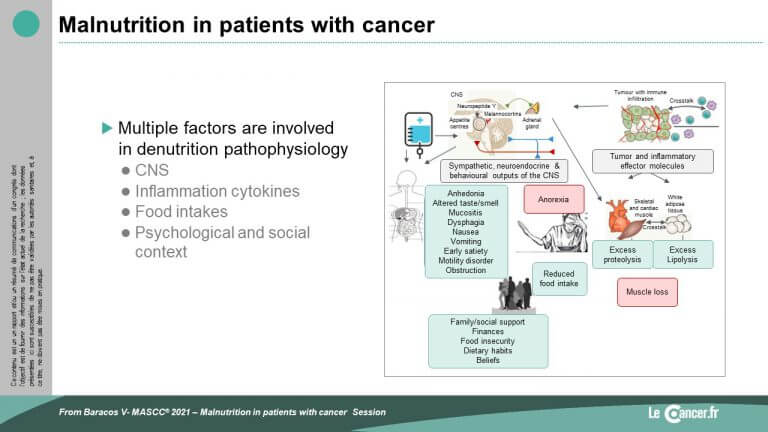
Malnutrition in patients suffering from cancer is multifactorial in origin: reduced intake (loss of appetite, taste, nausea, etc.), and above all complex inflammatory phenomena linked to the tumor, involving numerous cytokines and inducing hyper-catabolism. This results in weight loss and loss of muscle mass (sarcopenia), which leads to fatigue, reduced physical activity and, at an advanced stage, irreversible cachexia.
The first step is screening for undernutrition, which must be systematic, the idea being that an early diagnosis enables effective corrective measures to be put in place: measurement of weight, body mass index, assessment of intake, assessment of body composition (muscle mass and fat mass) by scanner, assessment of the context and favoring factors (nausea, pain, etc.).
An Italian study (Muscaritoli 2017) shows that at the time of cancer diagnosis, more than 30% of non-metastatic patients are at risk of undernutrition (compared with 50% in the case of metastases). The type of cancer also plays a role, with an additional risk in the case of digestive cancer, as well as certain treatments (radiotherapy of the esophagus, therapeutic intensification). The situation of elderly patients is even more worrying, with 65% of patients being malnourished according to some studies (Dunne 2019), as the decrease in functional capacity is clearly linked to survival in this population. Furthermore, weight loss can be very rapid, as soon as chemotherapy is started (Naito 2017).
The management of an undernourished patient, or one at risk of malnutrition, must be multidisciplinary. It is important to take into account all potential contributing factors, in particular other symptoms such as poorly controlled pain, diarrhea, constipation, mucositis and xerostomia (Charalambous 2017). The social context must also be taken into account: sufficient resources to have quality food intake, fight against isolation. Nutritional consultation is also important, enabling the qualitative and quantitative assessment of food intake, giving practical advice such as splitting up meals and maintaining the pleasure of eating.
Information for patients and their families is absolutely essential. Indeed, the management of a malnourished patient is based not only on their adherence to the proposed solutions but also on the follow-up elements that they will provide (PRO: Patient Reported Outcomes). Thus, adapted physical activity is useful and acts in synergy with nutrition to improve the patient’s physical condition (Kiss 2020).
With regard to drug treatments, it should be noted that Anamorelin, a Ghrelin receptor agonist (a molecule involved in the control of satiety) has just been authorized in Japan for cachexia in patients suffering from digestive or bronchial cancer.
The role of training doctors and carers was recalled, in order to make them aware of this problem which, if identified in time, can be the subject of effective measures.
Finally, it should be noted that a new ESPEN reference tool has been made available, in the form of decision trees that are easier to use in clinical practice and which concern not only patients undergoing treatment but also those who have been cured or are in the palliative phase.
Naito T. “Chemotherapy/Immunotherapy and Cachexia: Friend or Foe?” MASCC/ISOO 2021 Annual Meeting.
After cancer: What do cured patients die of?
This Australian retrospective study included more than 30,000 patients and confirms the clear cardiovascular excess risk of this population with more than 15% of fatal myocardial infarction.
Several studies have shown the increased cardiovascular risk for cancer patients. However, it is difficult to distinguish the short-term risk from the longer-term risk, which appears to be close to the general population.
The aim of this retrospective study was to assess the causes of death of patients living more than 5 years after cancer diagnosis and to compare mortality rates with those of the general population.
A total of 32,646 patients diagnosed between 1990 and 1999 were included. The mean age at diagnosis was 60 years and at death 81 years. The median follow-up was 17 years, and the most common cancers were: breast (19%), prostate (18%), skin (16%), and gastrointestinal (15%). Of the patients analyzed, 53% died.
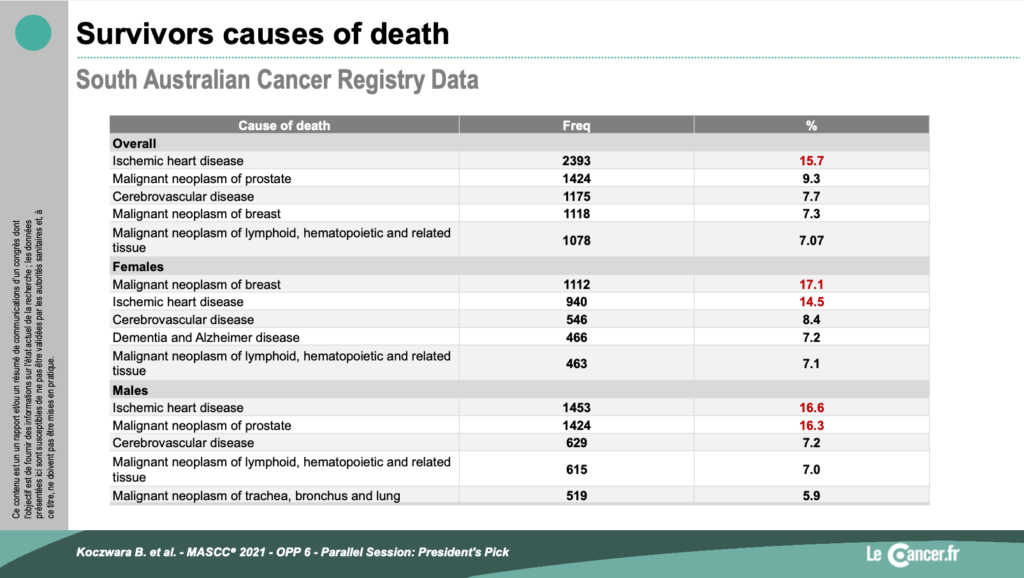
The most frequent causes of death were:
- for women: breast cancer (17%), ischemic heart disease (14%), stroke (8%), dementia (7%), hemopathy (7%)
- for men: ischemic heart disease (16%), prostate cancer (16%), stroke (7%), hemopathy (7%), ENT/lung cancer (6%)
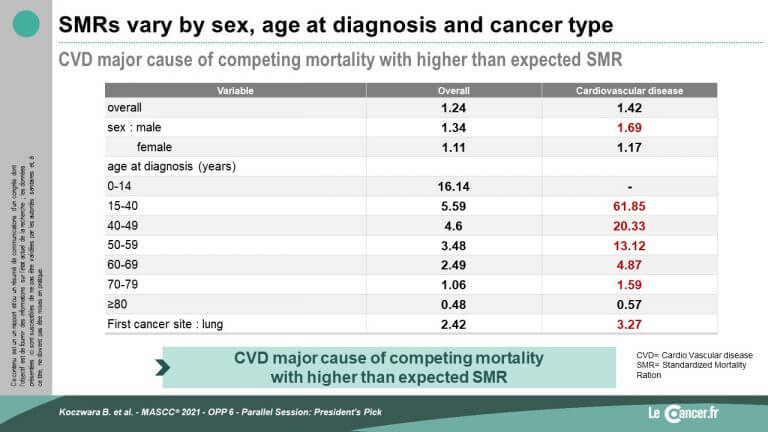
Survivor cancer patients most at risk of cardiovascular events were men diagnosed with lung cancer at less than 40 years of age.
Although conducted on a very large cohort, this study presents methodological biases: retrospective analysis, subjective reporting of causes of death in the registers, absence of data on pre-existing comorbidities.
In conclusion, this study undermines the idea that cardiovascular risk is reduced over time. This is a major post-cancer issue for these patients.
Koczwara B. “What Do Cancer Survivors Die of? An Australian Population-Based Study of Patterns of Late Mortality After Cancer.” MASCC/ISOO 2021 Annual Meeting.
Febrile neutropenia: The patient journey
Management of febrile neutropenia is feasible on an outpatient basis for patients at low risk of complications but primary prophylaxis with GCSF needs to be developed with possible use of pegfilgrastim and biosimilars.
The Febrile Neutropenia (FN) session opened MASCC 2021 with educational input from two leaders of the MASCC Febrile Neutropenia Study Group.
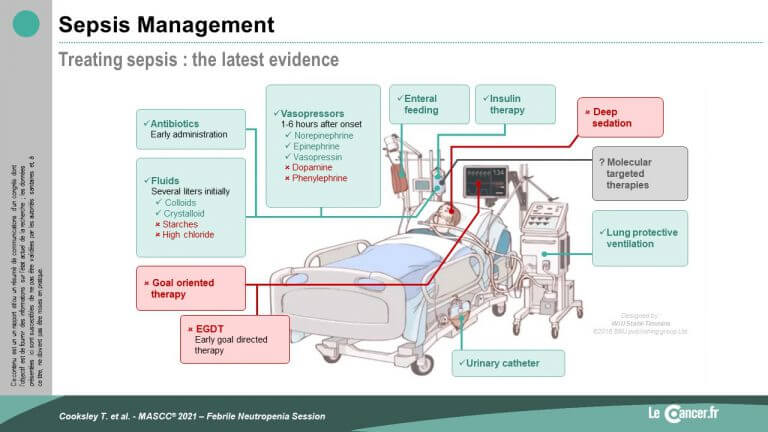
Tim Cooksley, from Manchester, gave an update on the management of sepsis related to febrile neutropenia and the importance of the most rigorous clinical, biological and imaging assessment possible. In addition to the use of volume support, antibiotics and vasoactive drugs, if necessary, he also highlighted the possible use of corticosteroids, particularly in the context of COVID-19 and rare but serious immune-related neutropenic complications.
He highlighted the possibility of using an ambulatory pathway for patients at low risk of complications, notably with a MASCC score ≥ 21 or a CISNE score 1 (low risk). This pathway is shown on the slide.
The use of G-CSF in curative settings was also discussed. Routine use of G-CSF to treat patients with febrile neutropenia is not recommended unless there is a risk of severe septic complications (poor prognostic factors, neutropenia likely to last more than 10 days and be profound (<0.1×109/L), uncontrolled primary cancer, age >65 years and organ failure, and onset of neutropenia during hospitalization). Fungal infection is also a high risk for curative G-CSF use.

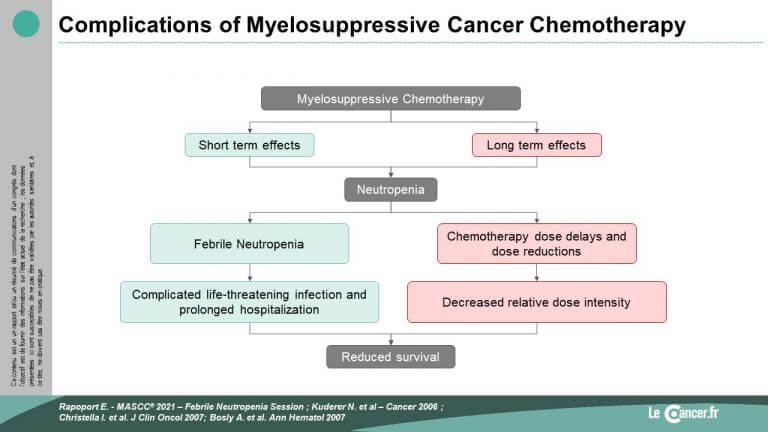
Bernardo Rapoport from South Africa, who also recalled the conditions of this recourse, then insisted on the importance of following the recommendations published in the context of febrile neutropenia, notably around prophylaxis. Febrile neutropenia impacts the survival of cancer patients, due to its acute complications but also due to the reduction of the relative dose intensity of the cancer treatments administered to our patients. The use of sustained-release forms of G-CSF (Pegfilgrastim) and its biosimilar forms has been emphasized, especially in the context of the COVID pandemic, in order to provide maximum protection to patients while limiting invasive procedures, pegfilgrastim being equivalent to approximately 10 days of filgrastim.


Cooksley, T. “Assessment and Diagnostic Work Up of a Febrile Neutropenic Patient.” MASCC/ISOO 2021 Annual Meeting.
Rapoport, B. “Management Strategies to Reduce Hospitalisation and the Role of Biosimilars in the Management of Febrile Neutropenia.” MASCC/ISOO 2021 Annual Meeting.
PRO: What benefit for immunotherapy?
This prospective and randomized study of patients treated for melanoma assessed the value of PROs in screening for immunotherapy-related toxicities.
The value of PROs (Patient Reported Outcomes programs) is well demonstrated in patients treated with chemotherapy or targeted therapy. What about those treated with immunotherapy?
The question deserves to be asked because of the particular profile of toxicities encountered with the immunotherapies currently used, i.e. checkpoint inhibitors (anti PD1/PDL1, anti CTLA4): broad spectrum potentially involving all organs, often non-specific clinical picture, impossibility of predicting these toxicities, very variable temporality.
This Danish study included 146 patients receiving immunotherapy in the adjuvant or metastatic setting. The patients were randomized between standard follow-up (medical consultation every 3 weeks, except in case of emergency) and PRO: in this case the patient had a tablet on which they reported a certain number of symptoms on a weekly basis, these being analyzed during the medical consultation. In the meantime, if a symptom worsened, for example, the software could advise the patient to contact the hospital.
The aim was to determine whether the occurrence of serious adverse events and, more generally, the number of adverse events and the use of healthcare resources (unscheduled consultations, telephone calls) could be reduced in this way.
The analysis of the results did not show any benefit on adverse events, neither in terms of severity nor incidence, nor on consultations, but the use of PROs did reduce telephone calls.
The use of PROs does not therefore seem to bring any benefit to patients undergoing immunotherapy.
It is also possible that the choice of symptoms monitored or the analysis every 3 weeks are not adapted.
Pappot H. “The Use Of Patient-Reported Outcomes To Detect Adverse Events In Metastatic Melanoma Patients Receiving Immunotherapy: A Randomized Controlled Trial.” MASCC/ISOO 2021 Annual Meeting.
Olanzapine vs metoclopramide in pediatrics
Olanzapine is more effective than metoclopramide for vomiting and nausea refractory to primary antiemetic prophylaxis in pediatrics.
A randomised open-label phase 3 study was conducted in a pediatric cohort of 80 children aged 5 to 18 years, treated with moderately to highly emetogenic chemotherapy. Primary prophylaxis was administered, combining a neurokinin type 1 inhibitor (aprepitant or fosaprepitant), a setron and a corticosteroid. Children included had at least one episode of vomiting despite a first dose of prophylactic antiemetic within 7 days of the last chemotherapy administration.

The primary endpoint was complete response, defined as no vomiting within 72 hours of initiation of olanzapine or metoclopramide.
Olanzapine and metoclopramide dosages were adjusted to the child’s weight.
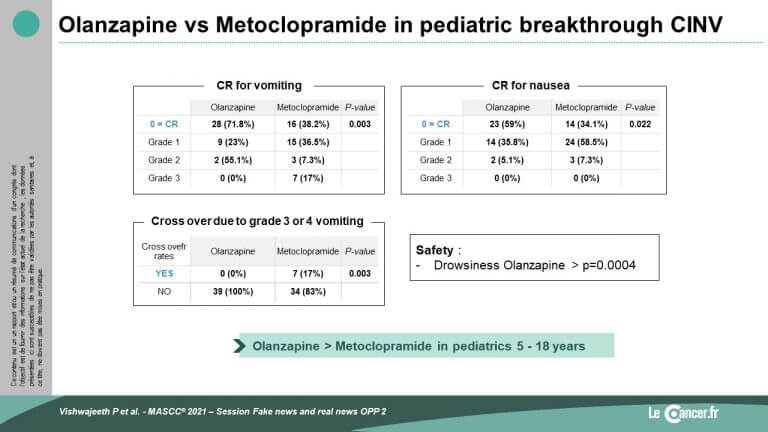
The results were significantly in favour of olanzapine for both the primary endpoint of vomiting (p=0.003) and the secondary endpoint of nausea (p=0.022).
Olanzapine was well tolerated, with no difference from metoclopramide apart from significantly greater somnolence with olanzapine.
In the cross-over study, the benefits were also in favour of olanzapine over metoclopramide on emesis (0% emesis vs 17%, p<0.001). It is important to note that a significant benefit (p<0.001) was found on nausea with the rescue use of both olanzapine and metoclopramide, compared to baseline.
Pai V. “Olanzapine Versus Metoclopramide For The Treatment Of Breakthrough Chemotherapy Induced Nausea And Vomiting In Children: A Randomized Phase 3 Trial.” MASCC/ISOO 2021 Annual Meeting.
Levorphanol: A new ambulatory painkiller
This exploratory study shows that Levorphanol could have a place in the therapeutic armamentarium as a second-line treatment for patients requiring opioid therapy.
Levorphanol is an old molecule, approved in the USA in the 1950s, with a potentially broad analgesic spectrum as it is a mu, kappa and delta opioid receptor agonist, NMDA receptor inhibitor and serotonin reuptake inhibitor. It can be taken orally, IV or subcutaneously, has a short onset of action (30 minutes) and a half-life of 11 to 16 hours, with a plasma steady state reached in 3 days. Its elimination is renal in the form of a glucuronide-conjugated active metabolite. Its undesirable effects are those of the opioid class, and its analgesic power is about 6 to 8 times that of morphine. In spite of this, and probably because of the priority given to other molecules, Levorphanol has been little evaluated and the clinical data concerning it are limited.
Reddy (MD Anderson, Houston) presented the results of an exploratory study, with the aim of determining the possibility of relaying with this treatment in patients on opioids and defining a conversion ratio.
Adult patients were treated with a strong opioid at a morphine equivalent dose of 60-300 mg/day and required opioid rotation.
Levorphanol was administered orally every 8 h, with an initial ratio of 1/10th of the morphine equivalent dose per 24 h. Painful episodes were also treated with Levorphanol. These patients were ambulatory, followed by telephone.
The conversion ratio took into account the possible use of an opioid in case of paroxysmal pain attacks with Levorphanol, if necessary.
Of the 40 patients included, 33 were able to be rotated, the other 7 patients were generally not related to Levorphanol. Tolerance was globally satisfactory, allowing a better efficacy and/or tolerance of the analgesic treatment. The conversion ratio was established at 8.5.
Levorphanol could therefore be an option for opioid rotation, in particular as an alternative to methadone. Prospective randomized trials are needed to confirm these results. Given the pharmacological profile of this molecule, its potential interest in neuropathic pain deserves to be explored.
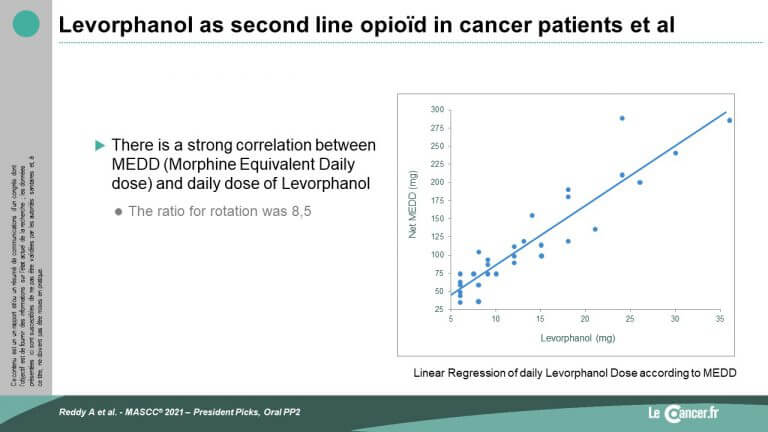
Reddy A. “Levorphanol as a Second Line Opioid in Cancer Patients Presenting to an Outpatient Supportive Care Center: An Open-Label Study.” MASCC/ISOO 2021 Annual Meeting.
GCSF Filgrastim IV or SC?
No difference in efficacy between intravenous and subcutaneous routes for injecting G-CSF in a retrospective study, but subcutaneous remains the recommendation due to study limitations.
Is there a difference between subcutaneous (SC) and intravenous (IV) use of filgrastim? A retrospective study compared the two approaches in a population of adult autologous non-Hodgkin’s lymphoma patients treated with chemotherapy (BEAM protocol). They were required to receive at least one injection of GCSF started at D5.
Time to neutrophil count >0.5×109/L was assessed. Secondary endpoints were duration of IV gram-negative antibiotic coverage, length of hospital stay and 30-day mortality. The two cohorts IV (94 patients) and SC (48 patients) were relatively balanced except for the higher creatinine level in the SC cohort.
The results showed no difference between the two routes of G-CSF administration, IV or SC, on either the primary (=0.93 – slide) or secondary endpoints:
- Duration of antibiotic therapy: p=0.20
- Length of hospital stay: p=0.24
- 30-day mortality: p=0.54
The limitations reported by the speaker were the lack of power of the study and its retrospective nature, as well as the difference in renal function between the two groups of patients. Finally, 17% of the patients in the subcutaneous cohort also received intravenous G-CSF compared to 0.2% subcutaneous in the intravenous cohort.
The question therefore remains as to how to limit pain and bleeding at the injection site, linked to the subcutaneous route, which remains the reference route in current international guidelines.
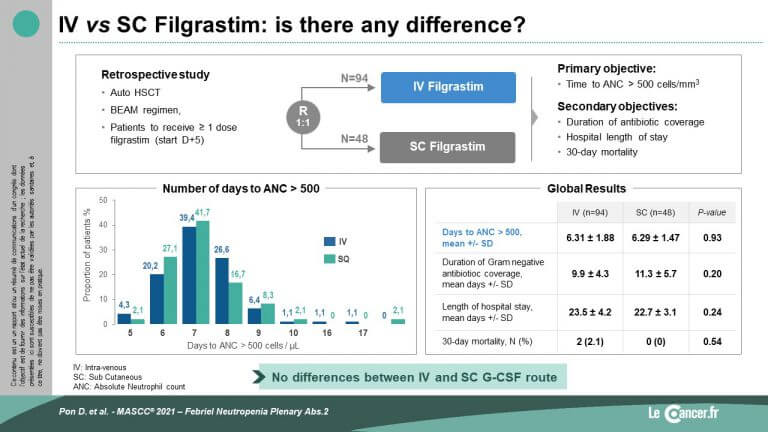
Pon D. “Comparison of Intravenous Piggyback (IVPB) versus Subcutaneous (SQ) Filgrastim in Autologous Hematopoietic – Stem Cell Transplantation (AUTOHSCT)”. MASCC/ISOO 2021 Annual Meeting.
One in three end-of-life cases is an ethical dilemma!
Decision-making for patients with advanced cancer at the end of life is in about 30% of cases a difficult choice between several morally acceptable options with no clear preference.
Incurable diseases involve the evaluation and consideration of many parameters such as refractory symptoms, the psychological impact of a decision, spirituality, the patient’s personal history, moral, social and cultural values, etc. Although oncological decision-making is governed by ethical principles, it often comes up against moral differences between the different parties in the end-of-life situation.
This Spanish multicenter, longitudinal, observational and prospective study included cancer patients with a life expectancy ≤ 6 months. The aim was to estimate the prevalence of ethical dilemmas at the end of life defined by a conflict in decision-making including the need to choose between several acceptable options without one standing out.
A total of 324 patients were included, mainly in hospital (56%) but also at home with a mobile palliative care team (22%). An ethical dilemma was observed in 28% of these cases.

In univariate analysis, there was a significant association between the occurrence of an ethical dilemma in care with gender (men, p<0.002), ongoing chemotherapy (p<0.035) and the presence of psychological distress (p<0.001).
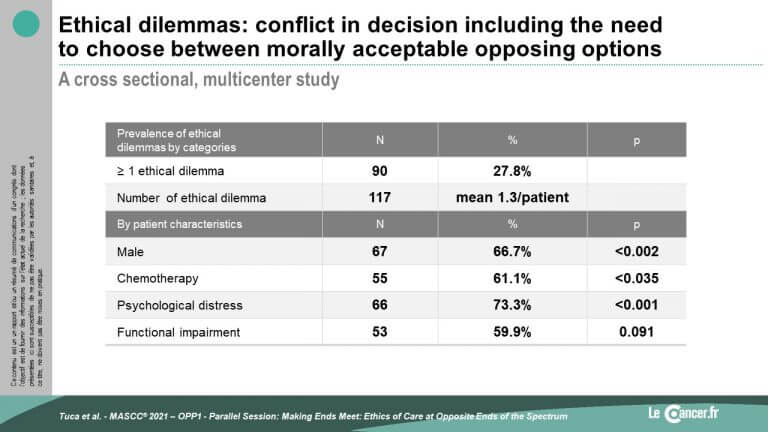

Conflicts were related to an information problem in 16% of cases, differences of opinion within the family (8%), between the patient or family and the medical team (4%), and within the medical team (4%). Requests for euthanasia concerned only 1% of the issues.

In conclusion, although this study reports a significant number of ethical dilemmas at the end of life, the divergences between carers and patients/families seem relatively small. It would be particularly interesting to anticipate possible points of divergence (announcement of incurability, unrealistic expectations, etc.) in order to limit these conflicts at the end of life.
Tuca A. “Prevalence of Ethical Dilemmas in the End-Of-Life Process of Advanced Cancer Patients”. MASCC/ISOO 2021 Annual Meeting.
What place for nursing in cancerology? A review of the scientific literature
The importance of the role of nursing in the management of cancer patients is emphasized, however nurses need to make progress in the reporting of their actions and missions.
Dr. A. Charalambous, President of the European Oncology Nursing Society (EONS), explains that theoretical concepts allow us to build nursing models. They are based on:
- a set of beliefs and values
- a statement of the goal that the nurse is trying to achieve
- the knowledge and skills the nurse needs to practice
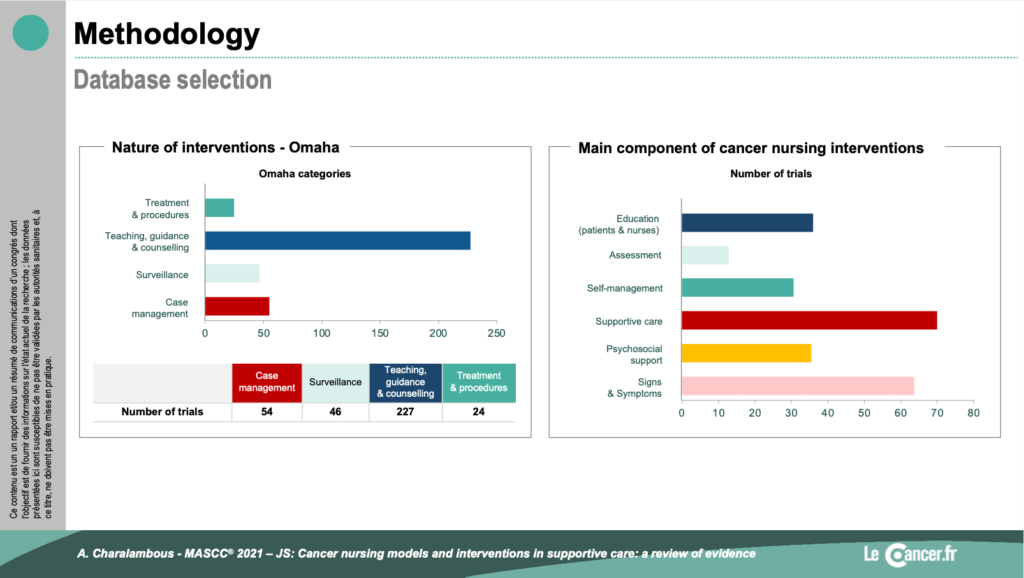
To understand the issue of oncology nursing, he analysed publications from 10 databases, published between January 2000 and June 2016. He extracted the data based on the TiDieR recommendations.
Most of the publications were from North America or Australia and a few from Europe. They are mainly in the context of curative treatment or in the post-cancer period. The effectiveness or otherwise of care by a cancerology nurse was not compared to any intervention (standard care): n=119 RCTs).
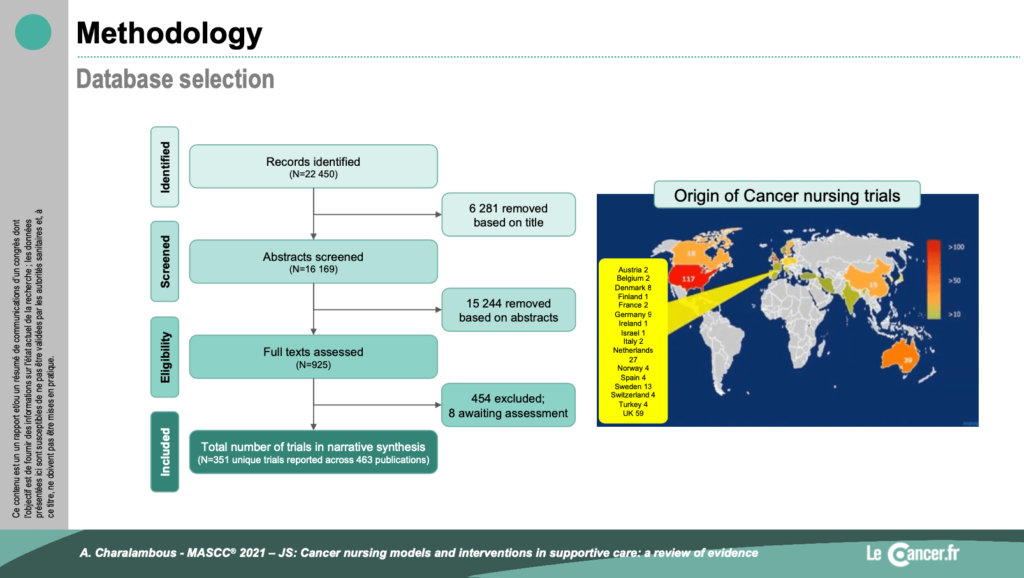
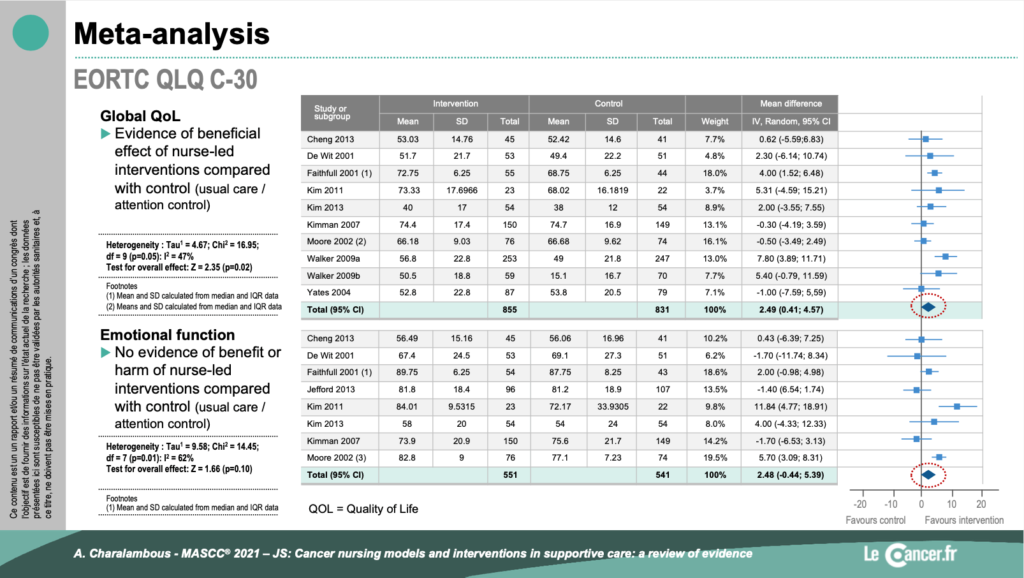
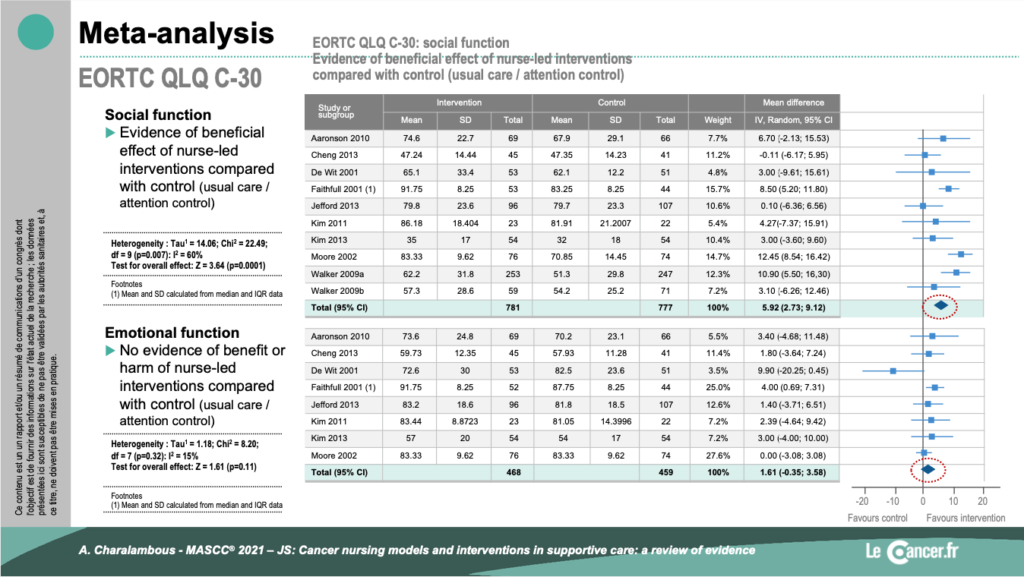
According to this analysis, the added value of management by an oncology nurse is important but variable. Indeed, it is not proven in all symptom areas but especially for quality of life and social care.
Nurses seem to show innovation and quality in their research but do not report their work sufficiently.
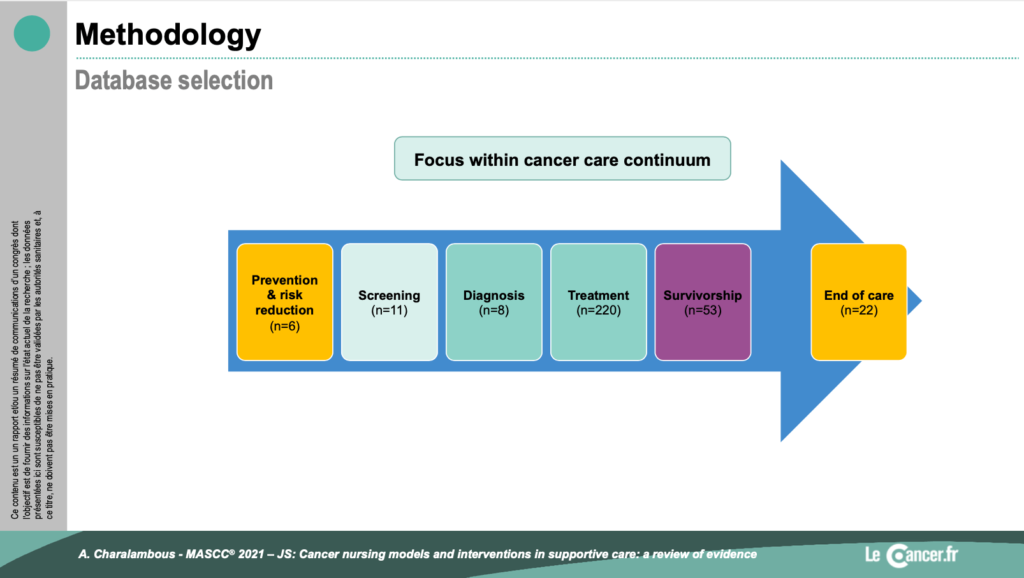
As Prof. Patsy Yates explained in her speech, the role of the cancerology nurses has grown over the years. This study confirms the added value of nursing care in oncology due to the construction of a nursing model of care based on caring values and a quest to achieve the goal of efficient care. However, there is still work to be done to enhance the role of nurses in the care of cancer patients.
Charalambous A. “Cancer Nursing Models and Interventions in Supportive Care: A Review of the Evidence.” MASCC/ISOO 2021 Annual Meeting.
Yates P. “Developments in the Role of Nurses in Providing Supportive Cancer Care Over the Past 40 Years.” MASCC/ISOO 2021 Annual Meeting.

